The Macrophages that could help fight Type 2 Diabetes
When we think about belly fat and type 2 diabetes, the story usually goes one way: excess fat causes inflammation, inflammation causes insulin resistance, and insulin resistance eventually leads to diabetes. But a new study from the University of Pittsburgh School of Medicine adds a surprising twist — and with it, a potential new path to treatment.
Not All Immune Cells in Fat Are the Enemy
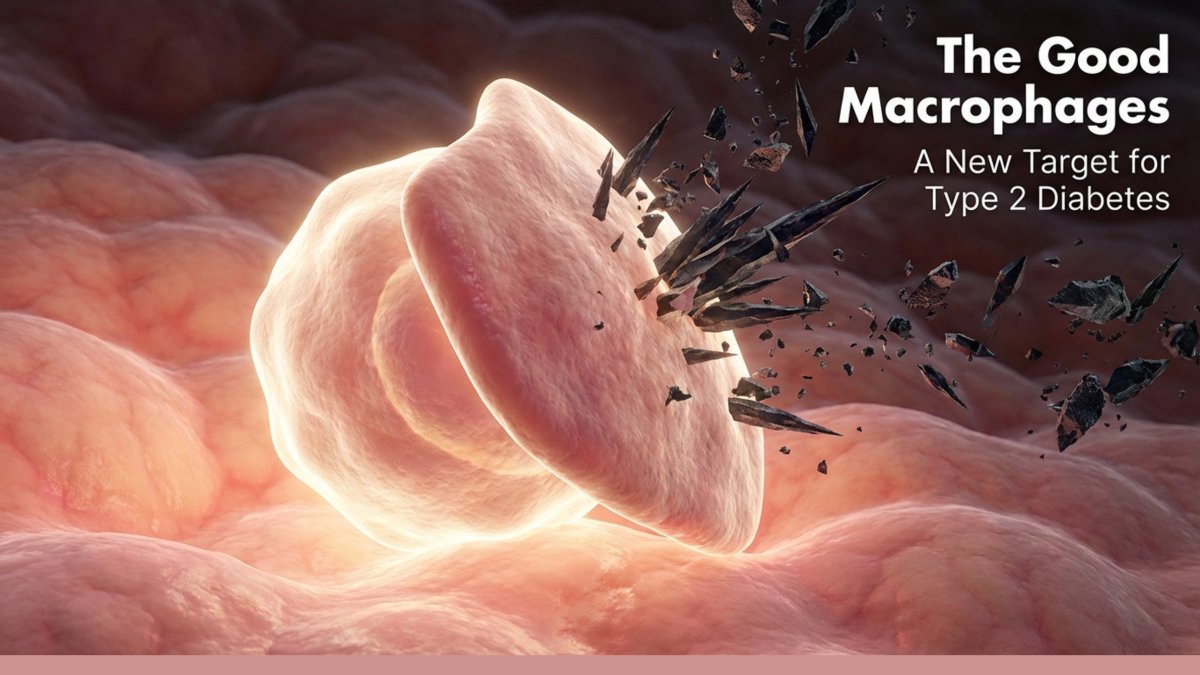
Researchers have long known that immune cells called macrophages accumulate in visceral fat (the fat stored deep in the abdomen around your organs) during obesity and drive inflammation. What was less understood is that not all macrophages are the same. The Pitt team, led by Dr. Partha Dutta, identified a distinct population of “resident” macrophages — cells that live long-term in visceral adipose tissue (VAT) — that actually do the opposite: they suppress inflammation and help keep fat tissue healthy.
“What we found is that there is a subset of immune cells in our fat tissue that are actually helpful,” said Dutta. “Although they’re immune cells, they’re not inflammatory — rather, they actually suppress the inflammation that causes insulin resistance.”
These VAT-resident macrophages are rich in mitochondrial antioxidant enzymes that keep inflammation in check and support normal insulin signaling. In a healthy state, they help the body stay metabolically balanced.
A Key Protein — and a Dangerous Spiral
The researchers discovered that a protein called SerpinB2 is essential for the survival of these protective cells. Under normal conditions, SerpinB2 levels are high in VAT macrophages, and the cells thrive. But when visceral fat accumulates — as it does in people who are overweight or obese — inflammation rises and SerpinB2 levels drop sharply.
The consequences cascade quickly. Without SerpinB2, the resident macrophages begin to die off. Without those protective cells, fat tissue becomes larger and increasingly inflamed. That inflammation then worsens insulin resistance, and blood sugar regulation deteriorates — setting the stage for type 2 diabetes.
In mouse models, selectively depleting these resident macrophages made glucose intolerance and insulin resistance measurably worse. Conversely, when the researchers administered antioxidant supplements to overweight, insulin-resistant mice, macrophage levels rebounded and insulin sensitivity improved.
A New Drug Target — and a Complement to GLP-1 Therapies
The findings, published in Nature Communications, point to SerpinB2 as a promising new therapeutic target. The team is now working to identify a small molecule that could boost SerpinB2 levels, protect resident VAT macrophages, and break the cycle of fat accumulation and inflammation before it leads to diabetes.
This approach could also prove valuable alongside existing GLP-1 weight-loss drugs like semaglutide. As Dutta noted, some patients on GLP-1 medications eventually plateau in their response. A therapy that targets the underlying immune dysfunction in fat tissue could complement these treatments — or help patients who no longer respond to them.
“Our goal is to develop a drug that will stop and reverse the process that leads to bad fat accumulation and insulin resistance by protecting and boosting the good immune cells that keep fat tissues healthy,” Dutta said.
Why This Matters
With roughly one-third of the global population classified as overweight or obese, and type 2 diabetes rates continuing to climb, finding new ways to address the root causes of metabolic disease is critical. This research reframes how we think about fat tissue — not just as a passive energy store or a source of harmful inflammation, but as an immunologically active organ with its own built-in defenses.
The study is still preclinical, and there’s a long road from mouse models to approved human therapies. But the discovery of a protective macrophage population in visceral fat, and the molecular key to keeping it alive, opens a genuinely new door in diabetes research.
Research published in Nature Communications by Partha Dutta et al., University of Pittsburgh School of Medicine, February 2026.
This topic was featured in Great News podcast episode 33.

The Great News Podcast is your source for positive news, inspiring stories, and good news from around the world. We skip the doom and gloom of mainstream media to focus on scientific breakthroughs, environmental wins, and the inspiring news that proves the world is getting better. Join Andrew McGivern for a dose of optimism and uplifting stories that will change your perspective on human progress.
It is easy to find the
Keep looking for the good in the world, because it is not only there – its everywhere.
Today we are diving into some truly groundbreaking developments in public safety, medicine, and clean energy.
What if I told you that despite what you see on social media, we are living in one of the safest times in history? That’s our lead story today.
Plus, we have a major update on the fight against cancer, a way to destroy ”forever chemicals” using nothing but sunlight, and a partnership that’s bringing advanced nuclear power to the grid.
America’s Crime Drop Is Real — And That’s Worth Celebrating
Canada’s Improved Cancer Survival Rate
Could Sunlight Be the Answer to “Forever Chemicals”The Next Generation of Nuclear Power Is Getting Closer to Reality
And don't forget to stick around for the speed round, where we'll dive into even more great news.70 People, 3,000 Cars: What Waymo Just Revealed About the Future of Self-Driving
The Battery Breakthrough Hidden in Plain Sight, Water
The Macrophages that could help fight Type 2 Diabetes
Making Hydrogen with Sun and Water?
And don't forget to follow the Daily Quote podcast. Kickstart Your Day in a Positive Way!

Source: Inside Precision Medicine